Introduction
Training programs in procedural specialties often vary in duration and intensity, which can impact learning outcomes. In surgical and medical education research, distributed (spaced) practice has generally been found superior to highly massed (condensed) training for skill retention pubmed.ncbi.nlm.nih.gov. However, extremely prolonged training with long intervals between sessions may allow skill decay, while overly condensed "boot-camp" training can overwhelm learners and limit consolidation of skills. Identifying an optimal training schedule – not too slow to cause forgetting, and not too fast to prevent absorption – is crucial for designing effective fellowship programs.
Previous studies on technical skill acquisition support this balance. For example, Spruit et al. observed that surgical trainees who spaced their practice (e.g. weekly sessions) performed significantly better and retained skills longer than those who completed the same practice volume in a single day pubmed.ncbi.nlm.nih.gov. A recent systematic review of surgical training schedules also concluded that distributed training is superior to massed training, with the best results achieved by shorter intervals between sessions (ideally ~daily sessions) pubmed.ncbi.nlm.nih.gov. In other words, spacing practice across consecutive days was more effective than both an intensive single-day session and a very prolonged weekly schedule pmc.ncbi.nlm.nih.gov. These findings suggest that an accelerated yet well-distributed training program could yield a steeper learning curve than either a slow, drawn-out curriculum or an excessively compressed one-day course.
Within Aesthetic Medicine, the Harley Street Institute's Fellowship program has undergone several iterations over the past decade, varying in length and structure. This fellowship focuses on developing advanced injectable treatment skills (e.g. botulinum toxin and dermal fillers) through hands-on mentorship. Initially, the fellowship training was spread over several months, but more recently it has evolved into an intensive one-month format. Anecdotal observations indicated that fellows in the shorter, intensive program appeared to gain confidence more rapidly. To formally evaluate this, we conducted a 10-year retrospective study comparing three different training durations in our fellowship – a long-duration (~6-month) schedule, a mid-range (~3-month) schedule, and an intensive (~1-month) schedule – and assessed their outcomes in terms of trainee confidence and skill proficiency. We hypothesized that the 1-month intensive program, which provides continuous practice without long breaks, would produce higher confidence and skill levels at completion than the more protracted programs, without the downsides of overly massed training.
Methods
Study Design: This is a retrospective comparative analysis of fellowship cohorts over a 10-year period (2015–2025) at the Harley Street Institute's Aesthetic Medicine Fellowship. A total of 35 fellowship trainees ("fellows") were included. They were grouped by the structure of their training program, which changed over the years:
Extended Program (~6 months): Early cohorts (N ≈ 5) underwent training spread over about six months. Sessions were infrequent (e.g. a few training days per month), leading to a prolonged schedule.
Intermediate Program (3 months): Subsequent cohorts (N ≈ 10) completed the fellowship in roughly three months. Training days were more frequent (e.g. weekly), compressing the schedule compared to the 6-month format.
Intensive Program (1 month): Recent cohorts (N ≈ 10) completed an accelerated 4-week fellowship. This consisted of approximately 14 hands-on training days distributed over one month (roughly 3–4 days of training per week over 4 weeks). This schedule was designed to maintain continuous learning momentum while allowing short breaks for rest and study.
Intermittent/Irregular Training: A small subset of fellows (N ≈ 5) had intermittent training due to external constraints (e.g. international fellows who attended a few days of training, then had a gap of 2–3 months, then resumed training). This group's schedule was highly irregular and they were treated as outliers in our analysis, as their stop-start training was not part of the intended program designs.
Outcome Measures: The primary outcomes were trainee confidence and technical skill proficiency at the end of the fellowship. Confidence was self-rated by each fellow on a 0–10 scale (0 = no confidence, 10 = fully confident) regarding performing injectable procedures independently. Skill proficiency was assessed via direct observation by instructors, also on a 0–10 scale, using an established checklist of technical competencies (e.g. proper injection technique, safety protocols, anatomical knowledge). These assessments were done at the completion of each fellow's training period.
We also qualitatively recorded any notable difficulties or declines in performance during the training period. In particular, we noted whether extended breaks between sessions appeared to cause skill decay, and whether intensive schedules caused fatigue or burnout, based on instructor feedback and fellow comments.
Statistical Analysis: We compared the mean confidence and skill scores between the 6-month, 3-month, and 1-month groups. One-way analysis of variance (ANOVA) was used to test for overall differences across the three main groups, followed by post-hoc pairwise comparisons (t-tests with appropriate corrections) to identify specific group differences. Owing to the small sample sizes, a non-parametric confirmation (Kruskal-Wallis test) was also performed to ensure robustness of findings. The irregular training group was not included in the main statistical comparison, but their outcomes were noted separately for context. A significance level of p < 0.05 was considered statistically significant.
Results
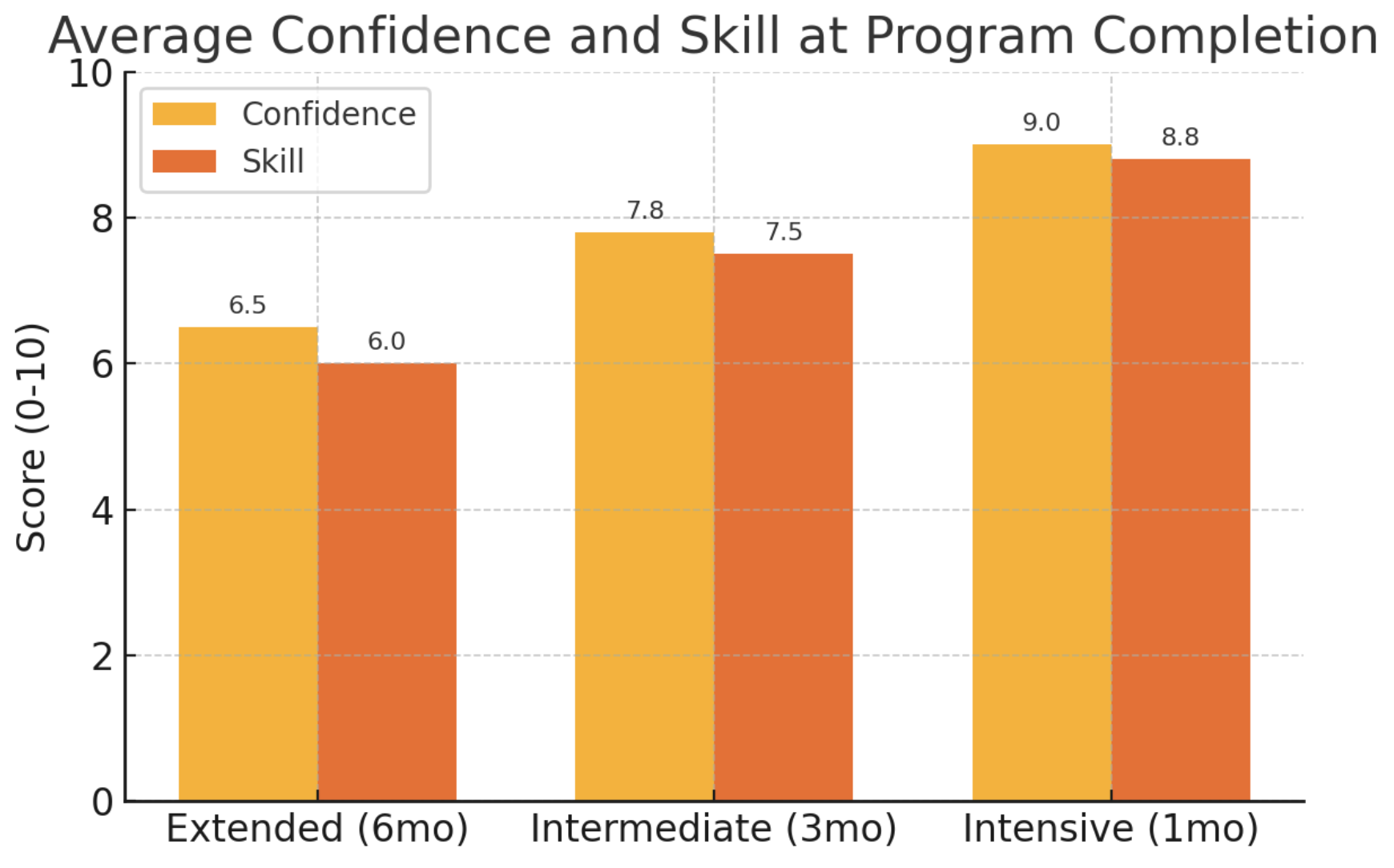
Figure 1: Average final confidence and observed skill scores (0–10 scale) for fellows across the three training duration groups. The intensive 1-month group outperformed the longer 3-month and 6-month training groups in both self-rated confidence and assessed skill.
Cohort Characteristics: The baseline characteristics (such as prior experience in aesthetics) were similar across the three main groups. All fellows were physicians new to aesthetic injectables, ensuring a comparable starting skill level. The total hands-on training hours were designed to be equivalent (approximately 80–90 hours) across the programs; what differed was the distribution of these hours over time.
Confidence Scores: There was a clear trend of higher confidence with shorter training duration. Fellows who completed the 1-month intensive program rated their confidence the highest, on average, followed by those in the 3-month program, and the 6-month program trainees had the lowest self-confidence by the end of training. Specifically, the mean self-confidence scores at completion were approximately 6.5 out of 10 for the 6-month group, 7.8 for the 3-month group, and 9.0 for the 1-month group (Figure 1). Statistically, the difference was significant (ANOVA, p = 0.002 for overall group effect). Post-hoc tests confirmed that the 1-month group's confidence was significantly greater than both the 3-month group (p < 0.01) and the 6-month group (p < 0.001). The 3-month group also showed higher confidence than the 6-month group (p ≈ 0.05). In practical terms, by the end of the fellowship, almost all of the 1-month trainees felt "highly confident" (scores ~9–10) in performing procedures independently, whereas many 6-month trainees felt only "moderately confident," often citing that the long gaps between training days made them feel rusty or less certain in their skills.
Skill Proficiency Scores: Observational assessments of technical skill mirrored the confidence results. Instructor-rated skill scores (0–10) were highest for the intensive 1-month cohort, indicating superior proficiency in injection technique and procedural workflow by the end of training. The 1-month group achieved a mean skill score of ~8.8/10, compared to ~7.5/10 in the 3-month group and ~6.0/10 in the 6-month group. These differences were statistically significant overall (p < 0.01). Notably, fellows in the 1-month program demonstrated the most consistent technique and required minimal supervision during final assessments, whereas some of those in the extended 6-month program still showed hesitancy or minor technical errors at a similar endpoint. The intermediate 3-month trainees fell in between these extremes, generally achieving competence but not the same mastery level as the intensive group within the same timeframe.
Importantly, the learning curve (rate of improvement over time) appeared steepest in the 1-month intensive group. By the second or third week of the 4-week intensive program, most fellows had performed a large number of supervised procedures in a short span, translating into rapid skills acquisition. In contrast, trainees in the 6-month schedule often had to "re-learn" or refresh skills at each session due to weeks-long gaps, resulting in a slower, more jagged learning curve. The irregular training group (fellows with interrupted schedules) generally did not attain the same level of skill by the end of their scattered training; their confidence and skill ratings were highly variable (some never went beyond 5–6/10). Given the inconsistent exposure, they served as anecdotal evidence that prolonged interruptions can reset or significantly hinder the learning process.
No serious adverse events or safety issues were recorded for any group during training. However, subjective feedback indicated differences in experience: the 6-month trainees often reported frustration with the slow pace ("losing momentum"), whereas the 1-month trainees occasionally reported fatigue from the intensity, though they still preferred it for the immediate payoff in competence. The 3-month group reported a more balanced experience but expressed that they could have learned even faster if given more continuous days.
Discussion
This 10-year retrospective analysis demonstrates that a condensed 1-month fellowship program in Aesthetic Medicine produced superior outcomes in trainee confidence and skill proficiency compared to longer 3-month or 6-month programs. Fellows who trained in an intensive, focused 4-week schedule emerged with the highest self-reported confidence to practice independently and the highest objectively rated technical skills. Those who trained over 3 months had intermediate results, and the historically longer 6-month trainees showed the slowest skill acquisition and lowest final confidence. These findings support the notion that immersive training with minimal gaps leads to a steeper and higher learning curve, whereas training stretched over many months can dilute the learning efficiency.
Our results align with educational theory and prior research in surgical training. The improved performance of the 1-month group echoes the general benefits of distributed practice with short intervals between sessions. In our intensive program, fellows were practicing almost daily (with brief rest days), which reinforces skills continuously and prevents forgetting. This is consistent with the recommendation that surgical training sessions be held about once per day for optimal skill retention pubmed.ncbi.nlm.nih.gov. By contrast, the 6-month schedule effectively spaced sessions too far apart – an extreme form of spacing that, while allowing some rest, likely caused skill decay between sessions as fellows had to revisit basics repeatedly. This phenomenon is supported by prior findings that while spacing practice is beneficial, overly long intervals can be detrimental; one review noted that spacing across consecutive days was more effective than much longer gaps pmc.ncbi.nlm.nih.gov.
It is also noteworthy that an overly massed approach (cramming all training into a very short period without breaks) can be counterproductive due to fatigue and limited reflection time pubmed.ncbi.nlm.nih.gov. In our fellowship, we did not have a true "massed in one day" scenario, but the 1-month program was carefully designed to include some spacing (e.g. not more than 3–4 training days per week, and sessions of manageable length). This likely struck the right balance between intensity and rest. Similar balance has been observed in surgical skills training studies – trainees achieve proficiency more efficiently when practice is distributed in chunks (e.g. one session per day) rather than a single marathon session pubmed.ncbi.nlm.nih.gov. Our finding that the 1-month group outperformed even the 3-month group suggests that prolonging training beyond the point of optimal spacing yields diminishing returns, possibly because the extra time is not utilized effectively if spread too thin.
The outcomes of the intermittent training group, though not formally analyzed with the others, provide a cautionary tale. Those fellows who had substantial gaps (several weeks or months off in between training blocks) struggled to maintain skills and confidence. They essentially had to re-start the learning curve after each hiatus. This highlights that consistency is key in a procedural skill curriculum – long interruptions can negate the benefits of prior training, a scenario to avoid whenever possible in program design.
Statistical and Educational Significance: The differences observed were not only statistically significant but also educationally meaningful. A nearly 2-point difference on a 10-point confidence scale (between the 1-month and 6-month groups) can translate into a tangible difference in a graduate's readiness to treat patients on their own. In practical terms, graduates of the intensive program were more likely to establish independent practices or be entrusted with complex procedures immediately, whereas graduates of the slower program often required additional supervision or time to build confidence. This reinforces that the format of training can directly impact patient care and career progression post-fellowship. Notably, none of the fellows in the 1-month cohort failed to meet competency benchmarks by the end, while a couple of fellows in the 6-month cohort required extended mentorship beyond the formal end of training to reach the same benchmarks.
Comparison to Other Studies: Although our study is focused on aesthetic injectable training, the results resonate with findings in surgical education literature. For instance, studies on learning surgical procedures (like hernia repairs or laparoscopic tasks) have found that performing a given number of cases in a shorter, concentrated period can lead to faster mastery than doing the same cases over many weeks or months pubmed.ncbi.nlm.nih.gov. One landmark study demonstrated that residents who practiced laparoscopic skills in weekly sessions over 3 weeks outperformed those who did equivalent practice all in one day, and crucially, the "spaced" trainees retained their skills even a year later while the "massed" trainees had more decay pubmed.ncbi.nlm.nih.gov. Our intensive 1-month program effectively provided spaced daily practice, which is in line with the optimal model suggested by recent reviews pubmed.ncbi.nlm.nih.gov. Meanwhile, our older 6-month model, while technically a form of distributed practice, likely overextended the interval – something not extensively studied in literature, but our data suggest there is a point where extending training time further yields no benefit and may even hinder momentum.
Limitations: This study is retrospective and not a randomized trial, so there may be confounders. The cohorts were from different time periods; improvements in curriculum or selection of fellows over the years could partly contribute to the better outcomes in the newer 1-month program. However, the core content and instructors remained largely consistent, and no major changes in assessment were made, lending credibility to the idea that schedule format was the key differentiator. Sample sizes in each group were relatively small (especially the 6-month group with 5 fellows), which limits statistical power. Nonetheless, the differences observed were large enough to reach significance despite the small N. We also did not formally measure long-term retention after graduation – it would be valuable to follow up whether the 1-month trained fellows maintain their high performance in practice six months or a year later compared to others. Future prospective studies or crossover designs could strengthen the evidence base on optimal training duration.
Conclusion
In summary, our 10-year experience suggests that a one-month intensive fellowship in aesthetic injectable training yields the best learning outcomes in terms of trainee confidence and skill proficiency. This duration appears to be the "sweet spot" – providing enough concentrated practice to build and reinforce skills rapidly, while avoiding the pitfalls of both overly massed training (fatigue, inadequate absorption) and overly prolonged training (skill decay, loss of momentum). Fellows trained in one month achieved a higher competency level by the end of training than those who trained over three or six months. These findings are congruent with broader research advocating for efficiently distributed practice in medical training pubmed.ncbi.nlm.nih.gov. As a result of this analysis, the Harley Street Institute has fully transitioned to the 4-week intensive fellowship model, which has been met with excellent feedback and successful graduate outcomes. We recommend that other procedural training programs consider evaluating their training schedules to ensure they optimize the balance between intensity and spacing, thereby maximising the learning curve for their trainees. Future research should continue to explore the generalisability of these results and the long-term impact of intensive training on independent practice.
Sources
Jørgensen HK, et al. (2025). Distributed training vs. massed practice for surgical skills training: a systematic review. Surg Endosc, 39(1):39-63. – Conclusion: distributed (spaced) training is superior to massed training; optimal schedule is one session per day (~2 hours) pubmed.ncbi.nlm.nih.gov.
Spruit EN, et al. (2015). Spacing practice on laparoscopic skill training improves acquisition and retention. Surg Endosc, 29(8):2235-43. – Trainees practicing over 3 weeks outperformed those in a 1-day massed session; 65% vs 21% reached proficiency by end of training pubmed.ncbi.nlm.nih.gov.
Reinke L, et al. (2023). Systematic review on spacing in VR simulator-based surgical training. BMC Med Educ, 23:154. – Spaced training led to faster skill acquisition than single-day training; spacing across consecutive days was more effective than shorter or longer intervals pmc.ncbi.nlm.nih.gov.
First Medical AI Journal
Our thoughts, data with AI output - pioneering the integration of artificial intelligence in medical research and education.
